|
Seed Implant Procedure (BRACHYTHERAPY)A seed implant is a simple outpatient
procedure that takes less than 1 hour. Men typically report to the hospital
in the morning, and return home a few hours later. The entire procedure is done through
very thin needles while under a light general anesthetic. There is no cutting involved and no stitches are
required. With an ultrasound in the rectum, a live picture of the prostate
is obtained. The Urologist then precisely places the needles in the prostate,
through the perineum (the area of skin between the scrotum and rectum). The Radiation Oncologist then inserts
the seeds through the needles. Once the procedure is completed and the anesthesia has
worn off, you can go home. Most men do not complain of pain and most do
not need a catheter after the procedure. Unlike surgery, the risk of incontinence is less
than 1%. Most men return to their normal activities the next day, and can return to work, playing golf,
etc.


Our Long-Term Outcomes with Seed Implant Based Treatment
Florida
Center for Prostate Care
|
| |
|
|
|
|
T1c-T2a,
Gleason ≤6, and PSA <10 |
|
|
|
T2b or Gleason 7 or PSA 10-20 |
|
|
High risk: only
1 risk factor |
T2c-T3,
Gleason 8-10, or PSA ≥20 |
|
High risk:
multiple risk factors |
T2c-T3,
Gleason 8-10, or PSA ≥20 |
|
|
Possible Side Effects Most men experience only temporary side effects
after the implant. Because there are no incisions or stitches required, there should only minimal discomfort after the brachytherapy
procedure. The most common complaint is temporary irritation of the urinary stream lasting only for a few months. It is common
to experience varying degrees of increased urinary urgency and frequency. Medications can be given to help alleviate these
symptoms. Long term side effects after the seed implant are very uncommon. Unlike surgery, 99% of men are continent and completely
able to control their urination. In addition, up to 90% of men treated with a seed implant can preserve their sexual potency
(ability to have erections). By precisely placing the seeds in the prostate with technique, the incidence of seed migration
outside the prostate is less than 1%. The likelihood of radiation causing any serious damage to any surrounding tissues outside
the prostate is consequently minimal in our hands.

What is Our Seed Implant Technique?
Why is it so important?
To have optimal results from your prostate seed implant, it is essential that all areas of the prostate
are covered with seeds, and that no sensitive areas outside the prostate are implanted. With our team’s technique and
experience, there is minimal risk of placement of needles or seeds too close to the bladder, rectum, urethra or nerves. Any
motion of the prostate or change in its size or shape during the procedure can be immediately taken into account, ensuring
perfect seed placement. Because seeds are precisely placed in the prostate, the risk of seeds migrating outside the prostate
is less than 0.4%.
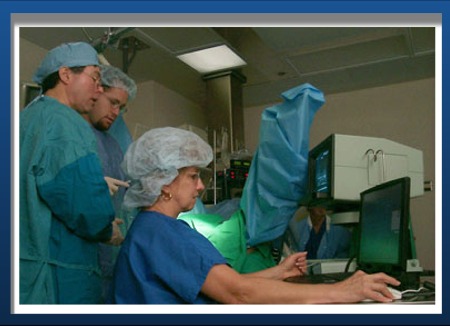
Our technique differs greatly from
the much older pre-planned, Dattoli, Prostrcision, or Mayo Clinic techniques. The pre-plan technique involves mapping out
the prostate a few weeks in advance by ultrasound. Then, when the patient goes to the operating room, the prior ultrasound
is used to determine where to place the needles and seeds. The pre-plan technique unfortunately does NOT take into account
any differences in the size, shape, or position of the prostate at the actual time of surgery. It has been our experience
that the prostate can be very different at the time of surgery. Subtle changes in leg position, the degree of bladder filling,
the use of anesthesia, and the shape of your prostate after the needles are inserted can have profound effects, making a pre-plan
virtually useless. In contrast, using powerful computers and experience based on thousands of previous cases, our teams technique
takes all of the above possible changes into effect. All of the needles and seeds are placed based on how the prostate looks
at the time of the procedure, not how it looked weeks before as pre-plan, Dattoli, Prostrcision, or Mayo Clinic perform. The
doses of radiation to the various areas are calculated live.

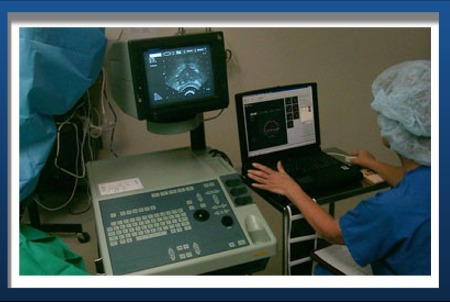
Intra-operative
computer planning Our physicians have helped pioneer the use of powerful computers during the implant
procedure to instantly calculate the dose of radiation received by the prostate and surrounding areas. The computer can obtain
and analyze live images of the prostate gland throughout the implant (brachytherapy) procedure to further ensure optimal seed
distribution and placement. This is a major improvement over older techniques where the amount of radiation received by the
prostate could not be determined until after all the seeds were implanted. Currently,
no other group in Florida is using this technique. 
Case for Combined Treatment For
treatment to be effective in patients who have more aggressive or advanced stages of prostate
cancer, it must be directed at both the prostate and the surrounding areas where cancer cells may have
spread. To accomplish this, a seed implant is typically combined with a
few weeks of IGRT (external radiation) and/or a temporary hormone blocking medicine. The seed implant delivers a high dose of radiation
to the prostate, where most or all of the cancer cells reside. The IGRT not only treats the cancer in the prostate, it also attacks cancer cells that may have spread outside the prostate. Hormone
blocking therapyProstate cancer typically feeds on testosterone, the male hormone.
A combination of a shot (Lupron or Zoladex) that you receive every few months from your
Urologist, and pills (Flutamide or Casodex) that you take daily can temporarily
block the testosterone in your body. By cutting off the "food supply"
to the cancer, several helpful things can happen: - After a few months, your prostate will shrink 30-40%
in size. In men with large prostate glands, it becomes easier to distribute
the seeds for the implant and fewer seeds are required. An added bonus
is that you will probably notice that it is easier to urinate because your prostate is smaller.
- Some
cancer cells outside the prostate may actually die, or "starve to death."
- The remaining cancer cells can be made more sensitive or vulnerable
to the upcoming radiation and thus more likely to be killed.
While hormone-blocking treatment
alone will not permanently rid the body of the cancer, it has been shown to improve cure rates with radiation in men with
more advanced stage cancer. It also has the ability to make the seed implant, also known as brachytherapy, procedure possible
in men with very large prostates that would have otherwise been technically too difficult to implant. When administered, men
typically take the hormone blocking treatment for two to three months before beginning radiation, and continue the treatment
until after the seed implant. Common side effects from the hormone blockers include temporary hot flashes, fatigue, and loss
of libido.

|